The Back Story
Ten months ago, I had surgery on my right foot and was told I’d be “good as new” in eight to twelve weeks. But twelve weeks came and went and pain was still my constant companion. It was infuriating! We had supposedly fixed the thing causing the pain (the bones rubbing together due to lack of cartilage), but here I was still aching each and every time I stepped on my right foot. I tried everything I could think of—acupuncture in the spring, cortisone injections in June—but nothing seemed to do the trick.
Physical therapy hadn’t been part of my prescribed recovery plan. In fact, my surgeon actively discouraged it, worried I’d get a bad practitioner. (A massage therapist, after all, was blamed for triggering my pain in the first place.) But as I ticked out of options to try, I decided physical therapy was worth a shot.
That’s how I ended up at Redbird Physio in Bend. They’d just opened a new location, which meant I could get in within a few weeks—a small miracle in itself here in Bend. Jen Mitol, the therapist assigned to me, was ten years my senior. We hit it off right away—probably because her quick wit and sense of humor reminded me a lot of my dear husband who’d just left for Baghdad. :)
Jen got to work and quickly ruled out any structural problems using a combination of manual manipulation and—surprisingly—a tuning fork. (Fun fact: touch a 256-hz tuning fork to a fractured bone and your body will let you know immediately.) The pain it produces is apparently unmistakable. Thankfully, that wasn’t my issue.
Still, I was terrified of having my foot touched. The pain had begun after a massage therapist dug too deeply into the ball of my foot, and even though she hadn’t caused the cartilage deterioration, my nervous system didn’t care about that distinction. I associated foot touching with pain which made me deeply distrustful of healing professionals—an inconvenient mindset when you’re actively seeking healing.
Jen saw my skittishness. She took things slow, building trust session by session. We spent three full sessions doing nothing more than gentle massage while I talked—about my history with Rheumatoid Arthritis, my anxious nature, my body-related panic attacks in my 20’s, and the caution I’d wrapped my body in since being diagnosed at seventeen. She took it all in and began building a plan. I didn’t know it at the time, but Jen was about to take me on a wild ride to retrain my brain and tackle this chronic pain for good!
The Issue
As Jen got to know my brain and body, she came to the conclusion that I was experiencing hyper-sensitization of the nervous system. It turns out that when your nervous system is hyper-sensitized, every sensory input—from chronic pain to temperature to inflammation—floods the brain with information that causes it to become overwhelmed. As a result, the brain gets confused, the normal checks and balances break down, and the accuracy of the information traveling between the brain and body becomes compromised.
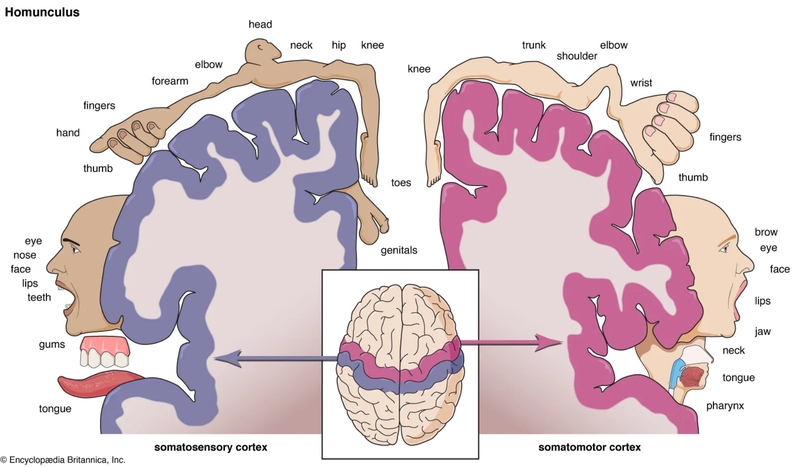
The part of the brain that gets its wires crossed due to sensory overload is called the homunculus. In simple terms, it’s a brain-based map of your body, where each section handles the sensory signals coming from a specific part of your body. If you’ve ever done a visualization where you’ve sensed into various parts of your body, then you, my friend, have called upon your homunculus!
Here’s the other thing you need to know about the homunculus. The more sensitive an area of the body is—like hands, lips and faces—the more brain real estate it takes up. That’s why the homunculus is often drawn as a funny-looking little person with huge hands and lips and tiny legs — emphasizing that it’s not about the body part’s actual size that matters, but about how much sensation your brain receives from that area.
One issue that can develop when the brain’s signals get mixed up is difficulty telling left from right in the painful body part. People with chronic pain often struggle to quickly and accurately identify whether images of that body part show the left or the right side. Compared to someone without pain, they may take longer or make more mistakes when making this distinction. Weird, huh?
Because of this, one of the first tasks Jen had me do was to download this app called Recognise Foot (Australian app, hence the weird spelling). The app showed me various images of feet from a multitude of angles and my job was to indicate whether it was a left foot or a right foot in two seconds or less. Here’s what it looks like on the app interface:
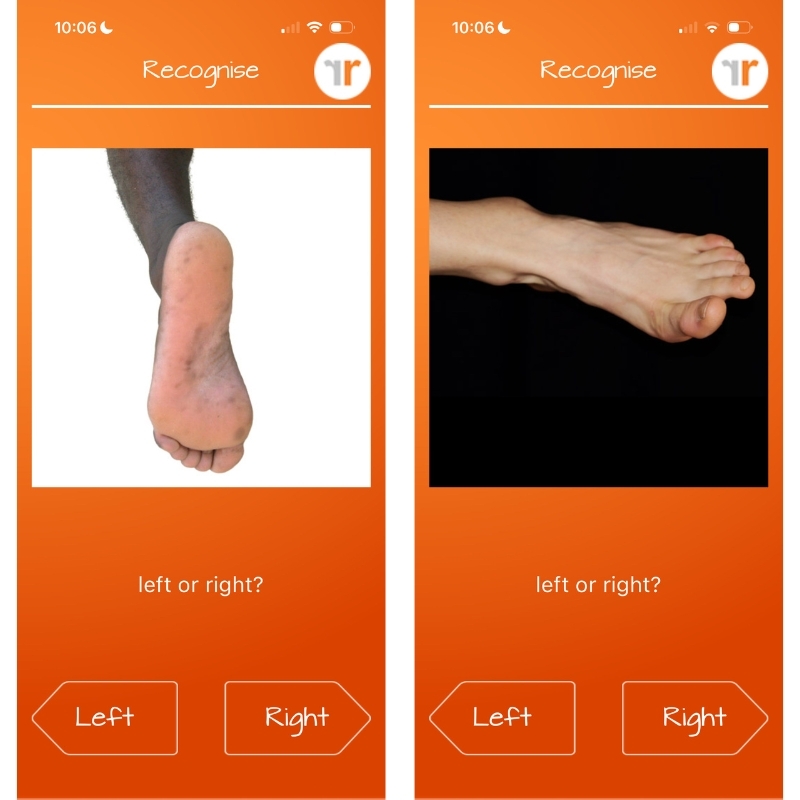
I was sure I’d nailed it. My results said otherwise:
Left-foot discrimination Percentage: 100%
Right-foot discrimination Percentage: 60%
Guess which foot was my injured one??
I was floored. In fact, I think I said to Jen, “You’re telling me that I can no longer tell what a right foot looks like?” This would be the first of many mind f’s to come. Here’s the good news though—the brain can be retrained, so after a week of app-playing each day, I was back to being able to discriminate right from left again!
The Body’s Warning System
Pain is meant to be a warning system that protects us from danger. Over time, my pain response system had become an overly sensitive alarm—like a smoke detector going off when toast burned. There was no real danger from the burned toast but the alarm thinks there’s a fire. The same thing is happening in my body. Because of my experiences with chronic pain, my anxious nature, AND the cautious way I viewed my body (Iike it was a fragile thing I had to keep bubble-wrapped), my internal pain alarm went off for the smallest things, amped up the volume even for trivial incidents, and often sounded when no real harm was happening.
Even when my foot injury was mostly healed, my brain and nervous system stayed on such high alert that normal touch, basic movement or simply thinking about my foot could bring pain. Here’s an interesting anecdote that proves my point: after writing Post 1 of this series on Monday night, I woke up the next day with an incredibly achy foot that was akin to how I felt two months post-surgery! I was amused that even now—10 months out of surgery, 4 months into PT—my brain still sounded the alarm when I spent too much time thinking about my foot. Fascinating, huh? You’ll be happy to know the pain resolved quickly, especially when I didn’t allow myself to get worked up about it.
When I began physical therapy, my activity level was almost nonexistent. I had to wear shoes at all times—complete with orthotic inserts—because walking on hard surfaces was simply too painful. I could manage short walks with minimal discomfort, but running or jogging was out of the question. Pickleball and exercise classes were still off-limits, as my foot couldn’t tolerate any high-impact movement. Yoga hurt. Hiking hurt. It was deeply frustrating, because while I don’t consider myself particularly sporty, I am very active—but after surgery I never saw the full recovery that I was promised.
So what do you do when pain slowly makes your world smaller and smaller? Contrary to what we’re often told, the answer isn’t to grit your teeth and push through it. Instead, real healing begins by helping your nervous system calm down and relearn what’s safe—by resetting the pain alarm back to its normal, protective level rather than letting it run the show.
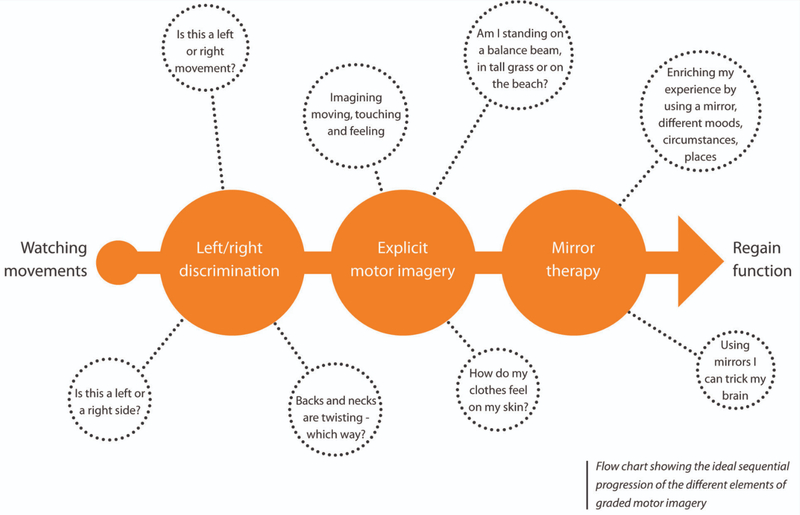
The Treatment: Graded Motor Imagery
Research has shown that the process of Graded Motor Imagery (GMI) is especially effective at retraining the brain. In essence, it’s a gradual (hence the graded part of the name) way of teaching the brain that movement is safe again without stressing the body part that’s already in pain.
There are three parts to GMI. As you might have guessed, left/right discrimination is the first. Once that is happening again, you move on to explicit motor imagery, then mirror therapy. The chart above details the desired progression. In my next (and hopefully last) post I’ll detail what that looked like for me.
In Part 2 I’ll delve deeper into the science and techniques Jen used to advance my healing. In the meantime, check out this fascinating podcast that does a really great job of explaining why we must target the brain to effectively reduce chronic pain. I hope you enjoy it!